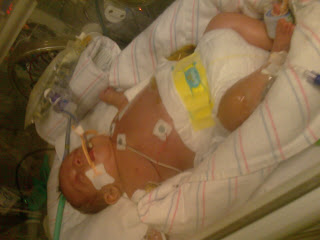
Mason continued to be unstable, he was NPO which meant he was not doing well at all, I hated these times. Not only was he dealing with those 2 chest tubes draining but he got a very bad infection. The infection started out in his urine but they started suspecting that his PICC line was infected. Without his PICC there was no way they could administer medication, we basically could not have an infected PICC it could be very dangerous as putting a new one in was not easy with Mason. His respiratory status was improving a bit but he was still draining about 290cc's, he was draining so much that they had to change the pediatric suction tubes to adult ones since they were replacing then very frequently. I did not understand why this was happening, I was confused did Dr. B not go in there to close the duct that was leaking all this fluid? I was so worried that I had to contact Dr.B myself. I went out of my way to email him I did not think I would get a response I emailed him on the 16th, 2 days went by and on the 19th I got a response back. He had a way of just calming me down, he didn't know just how much I trusted him. He always knew what to say, This was the response I got which made perfect sense. As you can see below Mason was very swollen.
Although I had heard from Dr. B I asked my social worker Jennifer who was always so great at helping me plan meetings with Masons doctors if she could schedule a meeting. I knew we were dealing with the chylothorax but this was something we might be dealing with for weeks. I wanted to start addressing Masons other problems. She actually managed to get me a meeting with Dr Strout, the head chief of the NICU. Yea he has a high position but had this Dr been following my babies care? We discussed some things with his cardiologist about discontinuing the INO and starting him back on Viagra. The only reason why Mason was on INO (Inhaled Nitric Oxide) was because he was NPO and Viagra was a PO medication. Once we could restart Mason on PO meds he could come off the INO. He agreed that as long as no residual was coming out of his repogle that they could try it. That's when this Dr gave me his opinion, he told me something I will never ever forget. He told me that I needed to start re-evaluating what I wanted to do for Masons life, and that there was going to be a time where they were not "Doing things for Mason, But just doing thing to Mason" and that I should consider taking him off life support. I was so offended, did this Dr not know how hard my baby had been fighting the last 4 months? Did he not know everything he had endured to that day? Did he not know that Mason had proved all the Miller Children's Dr's wrong? They have always questioned Mason and he has always proved them wrong..Why should I give up now cause some Dr that happens to run the NICU tells me too? I politely declined and the meeting ended. I stated my feelings to Masons primary as well to my social worker. I decided that day that I was going to stay with Mason, So I told the social worker to get me a family room....I was not leaving.
Mason was draining less which kept me so optimistic, Although everyone even his primary had hinted that maybe I should consider my options I did not want to give up. I had no right to just end his life because I felt he wasn't going to make it. When Mason decided he wanted to give up he would do so on his own, meanwhile I was going to continue to fight along with him...I kept in close touch with Dr.B, he was the only one who seemed positive and on our side, but then again Dr. B was a heart and thoracic surgeon and Mason had other issues he wasn't really aware of. The draining was minimizing, it still had not stopped but it was decreasing. I continued to be optimistic until on the 22nd we found out he had an infection, not only a gram zero bacteria infection but a PICC line, this was bad news as Mason only had a few IV's and required a lot of medication. He was beginning to decline so bad they started him on Epi, debutamin,dopamin and soluf cortef all to help with his blood pressure. He was not only on all the medication they could give him for blood pressure support he was reaching the max on his respiratory support as well. I had been staying with my husband in a family room in the NICU and I was checking in frequently, I had a real bad feeling. On the 23rd Mason was really critical, so critical that I called for a priest to baptize him in case anything happened. With no one allowed but my parents we went ahead and baptized him and asked them to be the God parents, All I wanted was for Mason to get Gods blessing in case anything happened.
I talked to one of the doctors and he wasn't too sure Mason could survive this infection but that they were trying the strongest antibiotics. We continued to stay in the NICUcc's that was way to much for any baby. Those days were very awkward, nurses started giving me the vibe that I was doing something bad by keeping my baby alive like this. Many nurses would tell me they felt sad to take care of my son? really? well because your sad I'm not going to let my son just die if I didn't know myself that he could maybe get over this and recover. I made that very CLEAR to his doctors as well as his primary. Jenna was a blessing from above, if we were going to continue fighting so was she, she contributed in every goal Mason met. We began to discuss a plan and we agreed that Mason needed a more stable central line. On the 27th I arranged another meeting to discuss the plan. Dr. B was at the conference which made me feel a lot better. We agreed that Dr. B would place a Jugular line on Mason to be able to get medications to him more effectively and quicker in case of emergency. We also agreed on Dr. B having to go yet again in to try and fix the chylothorax(the draining).On the 26th I went and got a tattoo, I just wanted to do it in his honor, I wanted to have him on me forever.
On the 27th Dr B placed a jugular line and immediately started octreotide (the medication to close the chylothorax) I was confident that by him getting it directly into his jugular it would make a better effect, Maybe I just wanted to reassure myself. I was doing countless of research and read that although it took some time this medication did work. Mason was draining so much that I was desperate for a solution, even if it meant him having to go into surgery again....I just knew we had to overcome this, we had come so far. The following day Mason drained 122cc's in 12 hours from both chest tubes, he was draining less and less...Was this a miracle? was he really getting better? or were the tubes just getting clogged(because they had gotten clogged in the past) I didn't get my hopes up, there was no way he could go from draining 300cc's to hardly nothing overnight. I began to worry so I emailed Dr. B
Once again, it was like this Dr was telling me everything I wanted to hear. He even agreed to order an Xray to check because I told him my concern about them being clogged. We had agreed on surgery the 29th if things were still bad but the 29th came and surgery got postponed. I couldn't believe it, we were actually getting over this.
Yes, we were on our way, It was a miracle and I happen to think that it had a lot to do with him getting babtized, he did not only get over Klebsiella a bacteria that should have killed him but his chylo was resolving. I felt beyond blessed. On April 30th one of the chest tubes came out....It was a great day, I was so proud, my baby was surviving after they pretty much assured me he was going to die. This was the 2nd half of April and we had just witnessed a miracle.
On the 27th Dr B placed a jugular line and immediately started octreotide (the medication to close the chylothorax) I was confident that by him getting it directly into his jugular it would make a better effect, Maybe I just wanted to reassure myself. I was doing countless of research and read that although it took some time this medication did work. Mason was draining so much that I was desperate for a solution, even if it meant him having to go into surgery again....I just knew we had to overcome this, we had come so far. The following day Mason drained 122cc's in 12 hours from both chest tubes, he was draining less and less...Was this a miracle? was he really getting better? or were the tubes just getting clogged(because they had gotten clogged in the past) I didn't get my hopes up, there was no way he could go from draining 300cc's to hardly nothing overnight. I began to worry so I emailed Dr. B
Once again, it was like this Dr was telling me everything I wanted to hear. He even agreed to order an Xray to check because I told him my concern about them being clogged. We had agreed on surgery the 29th if things were still bad but the 29th came and surgery got postponed. I couldn't believe it, we were actually getting over this.
Yes, we were on our way, It was a miracle and I happen to think that it had a lot to do with him getting babtized, he did not only get over Klebsiella a bacteria that should have killed him but his chylo was resolving. I felt beyond blessed. On April 30th one of the chest tubes came out....It was a great day, I was so proud, my baby was surviving after they pretty much assured me he was going to die. This was the 2nd half of April and we had just witnessed a miracle.